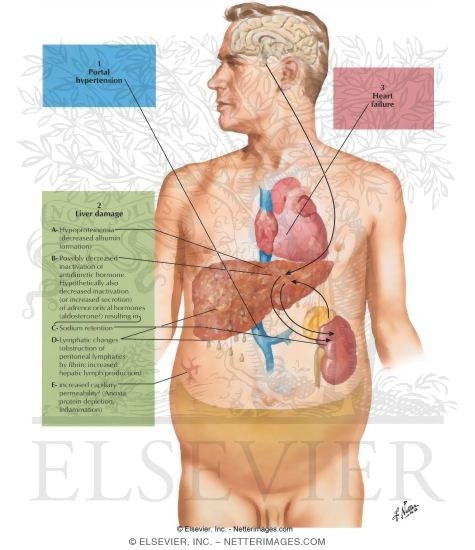
What is the treatment for ascites?
The treatment of ascites largely depends on the
underlying cause. For example, peritoneal carcinomatosis or malignant ascites
may be treated by surgical resection of the cancer and chemotherapy, while management of ascites
related to heart failure is directed toward treating heart failure with medical
management and dietary restrictions.
Because cirrhosis of the liver is the main cause of ascites, it will be the
main focus of this section.

Diet
Managing ascites in patients with cirrhosis
typically involves limiting dietary sodium intake and the
use of diuretics (water pills). Restricting dietary sodium (salt) intake to less
than 2 grams per day is very practical, successful, and widely recommended for
patients with ascites. In majority of cases, this approach needs to be combined
with the use of diuretics as salt restriction alone is generally not an
effective way to treat ascites. Consultation with a nutrition expert in regards to daily salt
restriction can be very helpful for patients with ascites.
Medication
Diuretics increase water and salt excretion from the
kidneys. The recommended diuretic regimen in the setting of liver related ascites is a combination of
spironolactone (Aldactone) and furosemide (Lasix). Single daily dose of 100
milligrams of spironolactone and 40 milligrams of furosemide is the usual
recommended initial dosage. This can be gradually increased to obtain
appropriate response to the maximum dosage of 400 milligrams of spironolactone
and 160 milligrams of furosemide, as long as the patient can tolerate the dose
increase without any side effects. Taking these medications together in the
morning is typically advised to prevent frequent urination during the night.
Therapeutic paracentesis
For patients who do not respond well to or cannot
tolerate the above regimen, frequent therapeutic paracentesis (a needle carefully is placed into the
abdominal area, under sterile conditions) can be performed to remove large
amounts of fluids. A few liters (up to 4 to 5 liters) of fluid can be removed
safely by this procedure each time. For patients with malignant ascites, this
procedure may also be more effective than diuretic use.
Surgery
For more refractory cases, surgical procedures may be necessary to control
the ascites. Transjugular intrahepatic portosystemic shunts (TIPS) is procedure
done through the internal jugular vein (the main vein in the neck) under local
anesthesia by an interventional radiologist. A shunt is placed between the
portal venous system and the systemic venous system (veins returning blood back
to the heart), thereby reducing the portal pressure. This procedure is reserved
for patients who have minimal response to aggressive medical treatment. It has
been shown to reduce ascites and either limit or eliminate the use of diuretics
in a majority of cases performed. However, it is associated with significant
complications such as hepatic encephalopathy (confusion) and even death.
Mor